Published in JACC
Introduction
Obesity and atrial fibrillation (AF) are dual epidemics that frequently coexist. Weight-loss reduces AF burden; however, whether this is sustained, has a dose effect or is influenced by weight-fluctuation is not known. The aim was to evaluate the long-term impact of weight-loss and weight-fluctuation on rhythm control in obese individuals with atrial fibrillation.
Material and methods
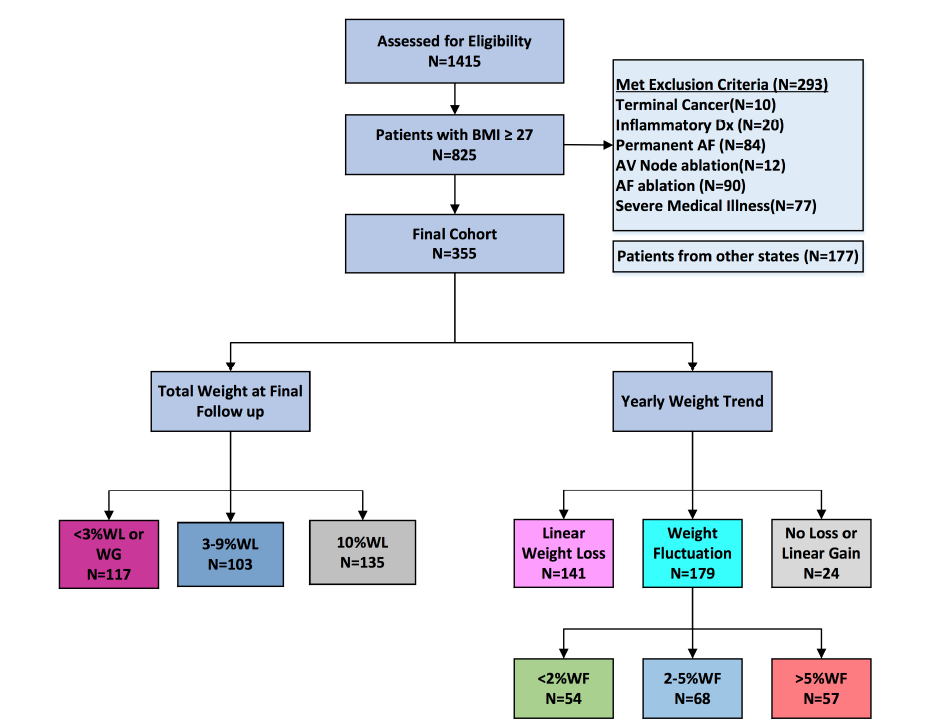
Figure 1: Flow chart
Of 1415 consecutive patients with AF (figure 1), 825 had BMI≥27 kg/m2 and were offered weight management. After screening for exclusion criteria, 355 were included in this analysis. To determine a dose-response, weight-loss was categorized as: Group-1 (>10%); Group-2 (3-9%); and Group-3 (<3%). Weight trend/fluctuation was determined by yearly follow-up. We determined the impact on AF severity scale and 7-day ambulatory monitoring.
Results
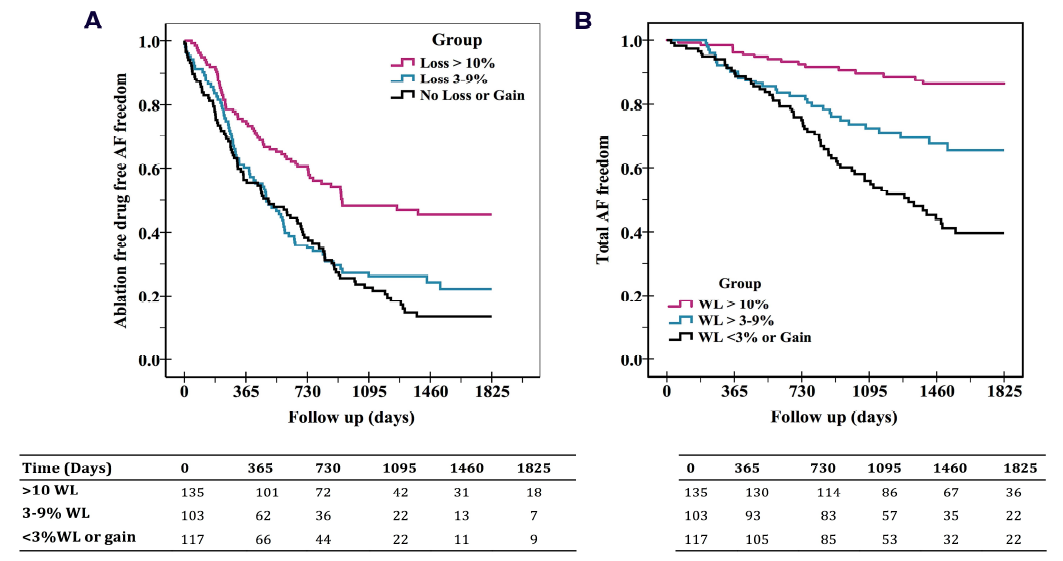
Figure 2A: Kaplan-Meier Curve for AF free survival without the use of rhythm control strategies. 2B: Kaplan-Meier Curve for AF free survival for total AF free survival
There were no differences in baseline characteristics or follow-up duration between the groups (p=NS). At follow-up, AF burden and symptom severity decreased more in Group-1 compared to Group-2 and 3 (p10% resulted in a six-fold (95% CI: 3.4-10.3, p<0.001) greater probability of arrhythmia-free survival compared to other two groups. Greater than 5% weight-fluctuation partially offsets this benefit with a two-fold (95% CI 1.0-4.3; p =0.02) increased risk of arrhythmia recurrence.
Conclusions
Long-term sustained weight-loss is associated with significant reduction of AF burden and maintenance of sinus rhythm. Weight-loss and avoidance of weight-fluctuation constitute important strategies for reducing the rising burden of AF.






